Glaucoma
Glaucoma is an eye disease that affects the optic nerve. Glaucoma often progresses without any symptoms, but it can cause permanent vision loss or blindness if left untreated. Therefore, it is extremely important to have regular eye exams to check for signs of glaucoma and other eye conditions. The glaucoma specialists at Eye Doctors of Washington provide advanced treatment options to effectively manage glaucoma, preserve vision, and prevent severe damage to the optic nerve. If you are seeking options for glaucoma management in Northern Virginia, Washington D.C, or Maryland, we can help. Contact us to schedule an appointment.
What is Glaucoma?
Glaucoma is characterized by optic nerve damage for which high pressure inside the eye is a major risk factor, although there are other factors in this complex condition. If the pressure in your eye is too high for an extended period of time, it can cause damage to the optic nerve – the nerve that connects the eye to the brain. When the optic nerve is damaged, you can start to lose vision. Glaucoma is a progressive disease, which means that it worsens with time. If glaucoma is not well-controlled, a person could ultimately lose all vision.
Types of Glaucoma
There are a variety of types of glaucoma, including very rare types such as congenital and juvenile glaucoma; the two main types of glaucoma are:
Open Angle Glaucoma
More than 95% of people with glaucoma have open angle glaucoma, so this is the type that is discussed most often.1 This type is also referred to as primary open angle glaucoma or POAG. In open angle glaucoma, the aqueous fluid within the eye can access the drainage system, but the drainage system itself does not function well.
Studies estimate that more than 3 million Americans have open angle glaucoma, but up to half of them do not even know that they have it.2 This is because open angle glaucoma often has no noticeable symptoms in the early stages. Since early detection is critical for managing glaucoma and maintaining vision, regular eye exams are important.
Narrow Angle Glaucoma
Narrow angle glaucoma occurs when the drainage system is blocked or obstructed by the iris (the colored part of your eye). When the aqueous fluid cannot drain out of the eye, the eye pressure will rise. If the eye pressure is too high for too long, optic nerve damage can occur, resulting in a loss of peripheral vision or ultimately total blindness.
This less common type of glaucoma is often considered a medical emergency and may be called a “glaucoma attack.” Symptoms of narrow-angle glaucoma include eye pain, blurred vision, headache, and nausea. You should see a medical professional immediately if you experience symptoms of narrow angle glaucoma.
Glaucoma Symptoms
The early stages of glaucoma are often asymptomatic. Symptoms of open angle glaucoma include blind spots in your vision and loss of peripheral (side) vision. Some types of glaucoma, such as narrow angle glaucoma, can cause headaches, halos around lights, or blurry vision. Glaucoma is progressive and by the time that symptoms are noticeable, the optic nerve has been damaged and any loss of sight may be irreversible. Glaucoma is a leading cause of blindness for people over 60 years of age, but glaucoma can be managed to prevent vision loss if it is diagnosed early.3
How is Glaucoma Diagnosed?
To make the diagnosis of glaucoma, our experts take into consideration a number of factors, including:
- The appearance of your optic nerves
- Your eye pressure
- The results of a number of diagnostic tests such as corneal thickness, nerve fiber thickness, and visual field testing
- Your medical history and other individual risk factors for glaucoma

In some patients, the diagnosis of glaucoma is very straightforward – the eye and optic nerve appear either very healthy or have clear signs of damage from glaucoma. On the other hand, some patients may have a number of concerning risk factors, eye findings, or test results that may or may not be related to glaucoma damage. In these cases, it takes time to diagnose the presence or absence of glaucoma with certainty, by determining if the optic nerve, visual field testing, or other diagnostic tests are changing (getting worse) over time.
Who Gets Glaucoma?
Anyone can get glaucoma, but it is most prevalent in people over 60. There are also some risk factors that may make you more likely to develop glaucoma, including:
- Family history of glaucoma
- African, Asian, Asian-Indian, or Hispanic heritage
- Nearsightedness (myopia)
- Diabetes
- High blood pressure (hypertension)
- Heart disease
- Lung disease
- History of eye trauma
- History of using corticosteroid medications
- Sleep apnea
- Very low blood pressure
- Inflammation in the body
- Hypothyroidism
- Migraine headaches
Lifestyle Changes to Prevent or Minimize the Effects of Glaucoma
It is critically important that you work with an experienced glaucoma specialist if you have, or are at risk for, glaucoma. Your eye doctor will discuss your treatment options, which will include medications or procedures to lower eye pressure. While there are no supplements, dietary changes, or lifestyle habits that can reverse glaucoma, there are some things you can do to care for your eye health, which may help control your eye pressure:
Develop Healthy Habits
Lifestyle choices that are good for eye health are also good for overall health. Regular aerobic exercise can lower eye pressure and improve oxygen delivery to the eyes. A balanced diet that includes a variety of vegetables and avoids excessive salt and added fats can support eye health.
Avoid Activities That Elevate Eye Pressure
If possible, avoid activities that can elevate eye pressure and blood pressure or constrict blood vessels, such as:
- Excessive caffeine intake
- Poorly controlled blood sugar or uncontrolled diabetes
- Diets high in trans fats or saturated fats
- Unmanaged hypertension
- Smoking
Glaucoma Treatment
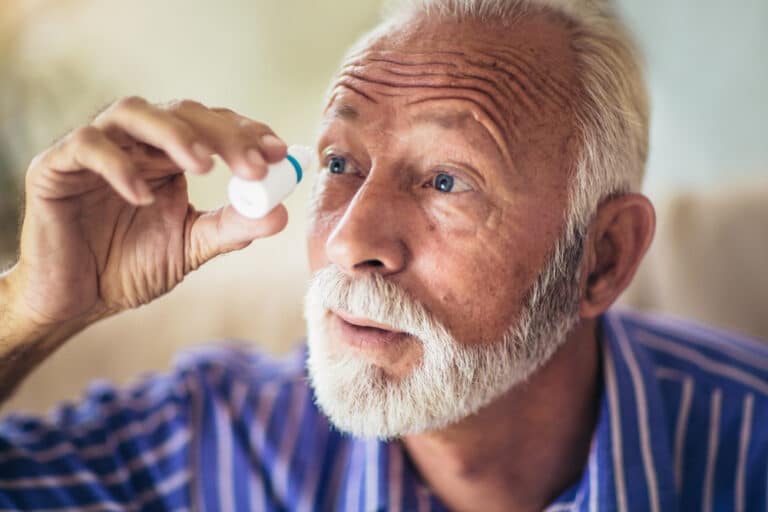
If you are diagnosed with glaucoma, the team at Eye Doctors of Washington will explain your treatment options and develop a plan to minimize damage to the optic nerve. Most treatments will aim to lower eye pressure. There is no cure for glaucoma, but a thorough treatment plan can control the condition with the goal of preventing vision loss.
Medications and Eyedrops for Glaucoma
There are several different types of medications and eye drops designed to manage glaucoma. These are often used as an initial treatment option and they are only effective if they are used consistently. If your glaucoma does not respond to medications or eye drops, your eye doctor may recommend you try a new treatment plan that could include different medication or a laser or surgical procedure.
Laser Glaucoma Treatments
Laser therapy can be used to treat glaucoma when medications or eye drops are not effective. It can also be used as first line therapy as well. Selective laser trabeculoplasty (SLT) is often used to treat open angle glaucoma. It works by improving the drainage system of the eye in order to lower pressure. Laser peripheral iridotomy (LPI) is a treatment used to prevent or treat narrow angle glaucoma.
Minimally Invasive Glaucoma Surgery (MIGS)
Minimally invasive glaucoma surgery, often called MIGS, is a highly advanced treatment option that uses microscopic-sized devices to improve fluid drainage within the eye. There are several types of MIGS, several of which are designed to be combined with cataract surgery.
Trabeculectomy
Trabeculectomy, also called glaucoma filtration surgery, is a surgical procedure to create a new drainage system within the eye. This surgery may be an option for patients who do not respond to other treatments or are not candidates for MIGS.
Aqueous Shunt
An aqueous shunt is a small device that is inserted to relieve high pressure in the eye. This procedure can be used to treat several types of glaucoma and it may be an option for patients who are not candidates for trabeculectomy. The aqueous shunt is a thin silicone tube with a small plate attached and it is designed to drain excess fluid to the plate, which acts as a reservoir. There are several types of aqueous shunts and your eye doctor will recommend one that is best suited to your needs.
Frequently Asked Questions About Glaucoma
What is considered normal eye pressure?
Keep in mind that eye pressure is an important risk factor, but it is not the only consideration in diagnosing glaucoma. There is no universally normal or safe eye pressure level that applies to everyone. A person can have higher than average eye pressures and not have glaucoma, or a person could have average eye pressures and have glaucoma. However, the average eye pressure level for most people is between 11 and 22 mg hg.
Is glaucoma hereditary?
If you have a family history of glaucoma, you are at a higher risk of developing the degenerative condition and it is often inherited from parent to child. However, there are a variety of factors that will influence your individual risk of glaucoma. This is why it is important for you to receive routine screenings to catch the disease as early as possible.
When should I get screened for glaucoma?
The American Academy of Ophthalmology recommends that everyone have a baseline eye exam at age 40 and then have exams every two to three years after that. Establishing your eye health will make it easier for your eye doctor to detect changes that could indicate a problem. You should have eye exams earlier and more often if you have risk factors for glaucoma or a history of eye conditions.
Can glaucoma damage be reversed?
No, optical nerve damage caused by glaucoma is permanent. This is why early diagnosis is crucial for protecting your vision. Once the disease is detected, your eye doctor can begin treatment immediately to help prevent further vision loss.
Contact The Eye Doctors of Washington for Glaucoma Treatment
The glaucoma specialists at The Eye Doctors of Washington are highly experienced in diagnosing and treating glaucoma. We offer comprehensive and personalized care and the most advanced treatment options. Contact us if you have any questions or if you are seeking a glaucoma management plan in Washington D.C., Northern Virginia, or Maryland.
1 BrightFocus Foundation. Glaucoma: Facts & Figures. Available: https://www.brightfocus.org/glaucoma/article/glaucoma-facts-figures Accessed August 17, 2020.
2 Friedman DS, Wolfs RC, O’Colmain BJ, et al. Prevalence of open-angle glaucoma among adults in the United States [published correction appears in Arch Ophthalmol. 2011 Sep;129(9):1224]. Arch Ophthalmol. 2004;122(4):532‐538. doi:10.1001/archopht.122.4.532
3 Mayo Clinic. Glaucoma. Available: https://www.mayoclinic.org/diseases-conditions/glaucoma/symptoms-causes/syc-20372839 Accessed August 17, 2020.





